- Published on
Meal Frequency and Glucose: Fasting vs. Snacking
Do you ever feel like you are constantly chasing your blood sugar levels throughout the day, snacking every few hours just to keep your energy steady? Or perhaps you have wondered if giving your body a break from eating could actually help you achieve better glucose control?
The debate between "frequent small meals" and "intermittent fasting" is one of the most common topics we discuss in the diabetes community. While everyone’s body reacts differently to food, understanding how meal frequency impacts your metabolic health is essential for finding a rhythm that works for you. Let’s explore the science behind these two approaches and how you can find your own balance.
The impact of meal frequency on your blood sugar
To understand why meal frequency matters, we first need to look at what happens in your body when you eat. Every time you consume carbohydrates, your body breaks them down into glucose (sugar), which enters your bloodstream. In response, your pancreas releases insulin to help your cells take in that glucose for energy.
When you eat frequently—say, every two or three hours—your body is in a near-constant state of processing food and secreting insulin. For some people, this approach helps prevent major dips in blood sugar. However, for others, it can lead to "glucose stacking," where your blood sugar levels never fully return to baseline before the next snack, leading to higher average levels throughout the day.
The case for consistent, balanced meals
Many traditional management plans suggest eating at regular intervals to prevent hypoglycemia (low blood sugar). This is particularly important for individuals on specific insulin regimens where timing is critical. If you choose this path, the focus should be on pairing carbohydrates with protein, fiber, and healthy fats to slow down digestion and keep your glucose curve flatter.
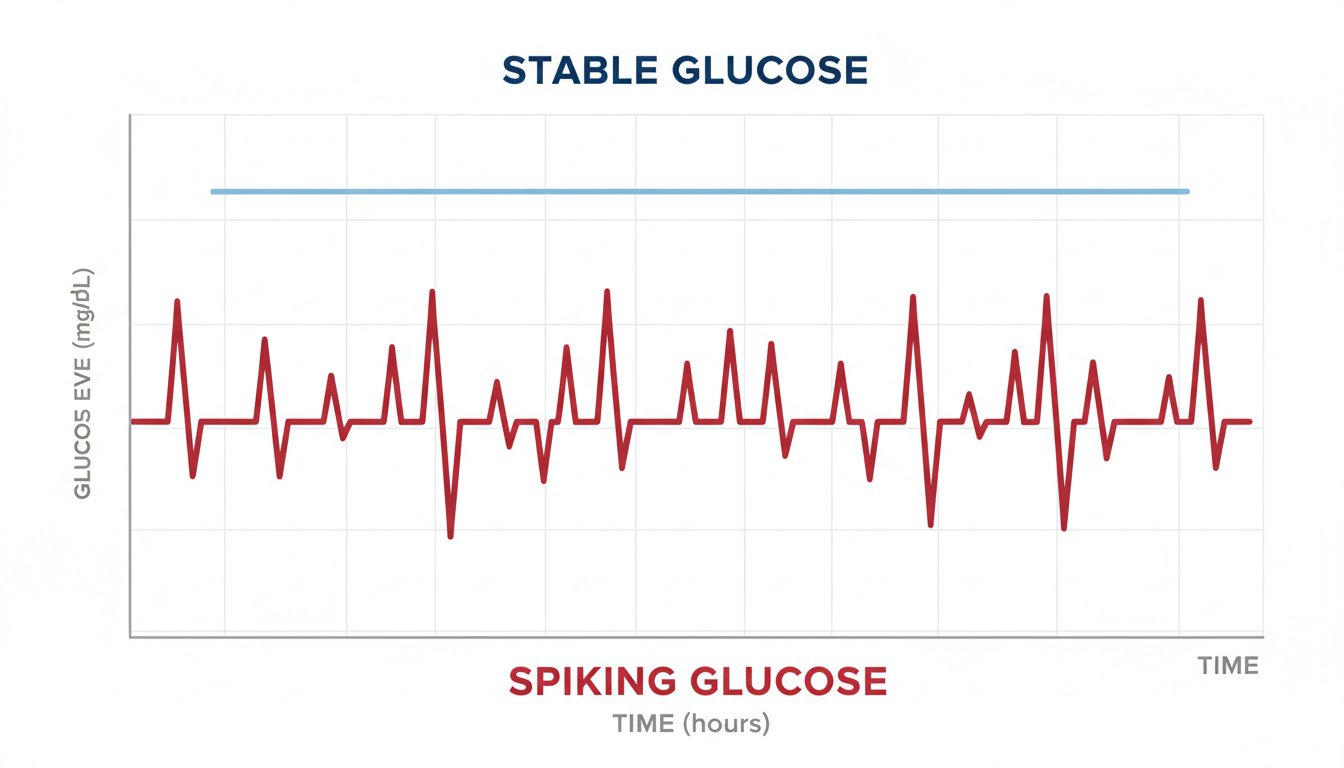
Exploring intermittent fasting for glucose stability
Intermittent fasting (IF) has gained popularity because it flips the traditional "eat often" model on its head. By restricting your food intake to a specific window of time—for example, the 16:8 method, where you fast for 16 hours and eat within an 8-hour window—you give your digestive system and your insulin levels a chance to reset.
When you are not eating, your insulin levels drop significantly. This allows your body to tap into stored energy and can improve your insulin sensitivity—how effectively your cells respond to insulin. For many, this leads to more stable blood sugar levels during the fasting period and a reduction in the total number of glycemic excursions (spikes) throughout the day.
Is fasting right for you?
It is important to note that fasting is not for everyone. If you take insulin or certain medications that lower blood sugar, fasting can increase the risk of dangerous lows. Before making any significant changes to your meal timing, please consult your doctor to ensure it is safe for your specific health profile.
Identifying your personal rhythm
Whether you choose frequent, smaller meals or a fasting window, the most important metric is how your body responds in real-time. What works for one person might cause a spike for another. This is where tracking becomes your greatest asset.
By using tools like a Continuous Glucose Monitor (CGM)—which tracks your glucose levels automatically throughout the day—you can observe exactly how your blood sugar reacts to the timing of your meals. Are you seeing "stair-stepping" spikes when you snack? Does your glucose stay flatter when you skip a mid-morning snack?

How to use data to find your balance
If you are interested in experimenting with your meal frequency, try these steps:
- Keep a food log: Use a tool like GlucoAI to record when you eat and what you eat. Seeing your meals side-by-side with your glucose data is a game-changer.
- Observe the "baseline": Look at your glucose levels before you eat your first meal of the day. Does a longer fast result in a more stable morning reading?
- Analyze the post-meal curve: If you are snacking, look at your data 2 hours after your snack. Are you still elevated, or have you returned to your target range?
- Consistency is key: Don't change your timing and your food choices at the same time. Keep your meals consistent for a few days while changing only your frequency to see the true impact.
For more on how to interpret these trends, check out our beginner's guide to interpreting CGM data.
Troubleshooting common challenges
"I feel shaky when I try to fast"
If you experience shakiness or dizziness, your blood sugar may be dropping too low or too quickly. This is a sign to break your fast and perhaps re-evaluate your intake. Try incorporating more protein or healthy fats in your last meal of the day to promote satiety and stability.
"I find it hard to stick to a schedule"
Life is unpredictable. If you have a busy day, focus on the quality of your meals rather than the clock. Even if your meal timing shifts, pairing carbohydrates with fiber (as discussed in our article on fiber intake) can help stabilize your glucose regardless of when you eat.
Results you can expect
When you find the meal frequency that keeps your glucose in range, you will likely notice more than just better numbers. Many people report:
- Increased energy: Fewer spikes and crashes mean less fatigue.
- Reduced cravings: When your blood sugar is stable, you are less likely to experience the "hangry" feelings that lead to impulsive snacking.
- Better A1C (average blood sugar level over 3 months): Consistent, stable daily numbers contribute to improved long-term outcomes.
Summary and next steps
There is no one-size-fits-all approach to how often you should eat. For some, frequent, smaller meals keep their glucose level; for others, the reset of intermittent fasting provides better stability. The key is to move away from guesswork and toward data-driven decisions.
- Start by tracking: Use a glucose tracking app to monitor your current habits for one week without changing anything.
- Analyze your data: Look for patterns where snacking might be causing your glucose to stay elevated.
- Consult your care team: Always discuss major changes in meal timing with your doctor, especially if you are on medication.
- Refine your approach: Use the insights from your logs to adjust your window or meal frequency, focusing on what keeps your time-in-range highest.
Managing blood sugar is a journey, not a sprint. If you are looking for a way to make sense of your glucose patterns, GlucoAI can help you visualize your data and identify which meal habits work best for your unique metabolic health. Start tracking your meals and glucose today—small, consistent adjustments are the most sustainable path to long-term health.
GlucoAI — Smart Blood Sugar Monitor
Track, analyze, and optimize your glucose levels with AI-powered insights.