- Published on
Preventing CGM Compression Lows for Better Sleep
It’s 3:00 AM. You are deep in a restorative sleep when suddenly, a piercing alarm shatters the silence. Your heart races as you fumble for your phone or receiver. The screen flashes a terrifying number: 55 mg/dL. Panicked, you perform a mental scan—do you feel shaky? Sweaty? Confused? You feel perfectly fine, albeit exhausted. You head to the kitchen, prick your finger for a manual check, and the meter reads a stable 102 mg/dL.
If this scenario sounds familiar, you’ve experienced the "compression low." For many in the Continuous Glucose Monitor (CGM) community, these false alarms are a significant hurdle to achieving quality sleep and maintaining metabolic health. While CGMs are revolutionary tools for diabetes management, they aren't perfect. Understanding the mechanics of compression lows is the first step toward reclaiming your nights and trusting your data again.
What Exactly Is a Compression Low?
To understand a compression low, we first need to look at how your CGM actually works. Unlike a traditional finger-prick meter that measures glucose in your blood, a CGM measures glucose in the interstitial fluid—the fluid that surrounds your cells.
When you lie down on your sensor, the physical pressure of your body weight pushes the interstitial fluid away from the area where the sensor’s tiny filament is located. Because there is less fluid for the sensor to "read," the glucose concentration appears to drop rapidly. It’s not that your actual blood sugar has plummeted; it’s simply that the sensor has been temporarily deprived of the medium it needs to provide an accurate measurement.
Think of it like a garden hose. If you step on the hose, the water flow at the other end drops to a trickle. The water pressure in the main tank (your blood) hasn't changed, but the delivery to the nozzle (the sensor) has been restricted. As soon as you roll over and remove the pressure, the fluid rushes back, and your readings usually return to normal within 10 to 15 minutes.

Why Compression Lows Are More Than Just an Inconvenience
At first glance, a false alarm might seem like a minor annoyance, but the ripple effects on your health can be profound.
1. Alarm Fatigue
When your device cries wolf too many times, you may begin to suffer from alarm fatigue. This is a dangerous psychological state where you start to subconsciously ignore or silence alerts because you assume they are false. If you have a genuine nighttime hypoglycemic event (low blood sugar) and your brain has been trained to ignore the alarm, the consequences can be severe.
2. Sleep Fragmentation
Quality sleep is a cornerstone of metabolic health. Every time a compression low wakes you up, your body releases cortisol (the stress hormone) to help you deal with the perceived emergency. Elevated cortisol can lead to insulin resistance the following day, making your blood sugar harder to manage. Continuous sleep disruption is linked to higher A1C levels and increased cardiovascular risk.
3. Over-Correction
One of the biggest risks of a compression low is "treating" a number that isn't real. If you are half-asleep and see a 60 mg/dL on your CGM, you might reach for glucose tabs or juice without confirming with a finger prick. This leads to a massive, unnecessary spike in the morning, creating a "rollercoaster" effect that leaves you feeling sluggish and frustrated.
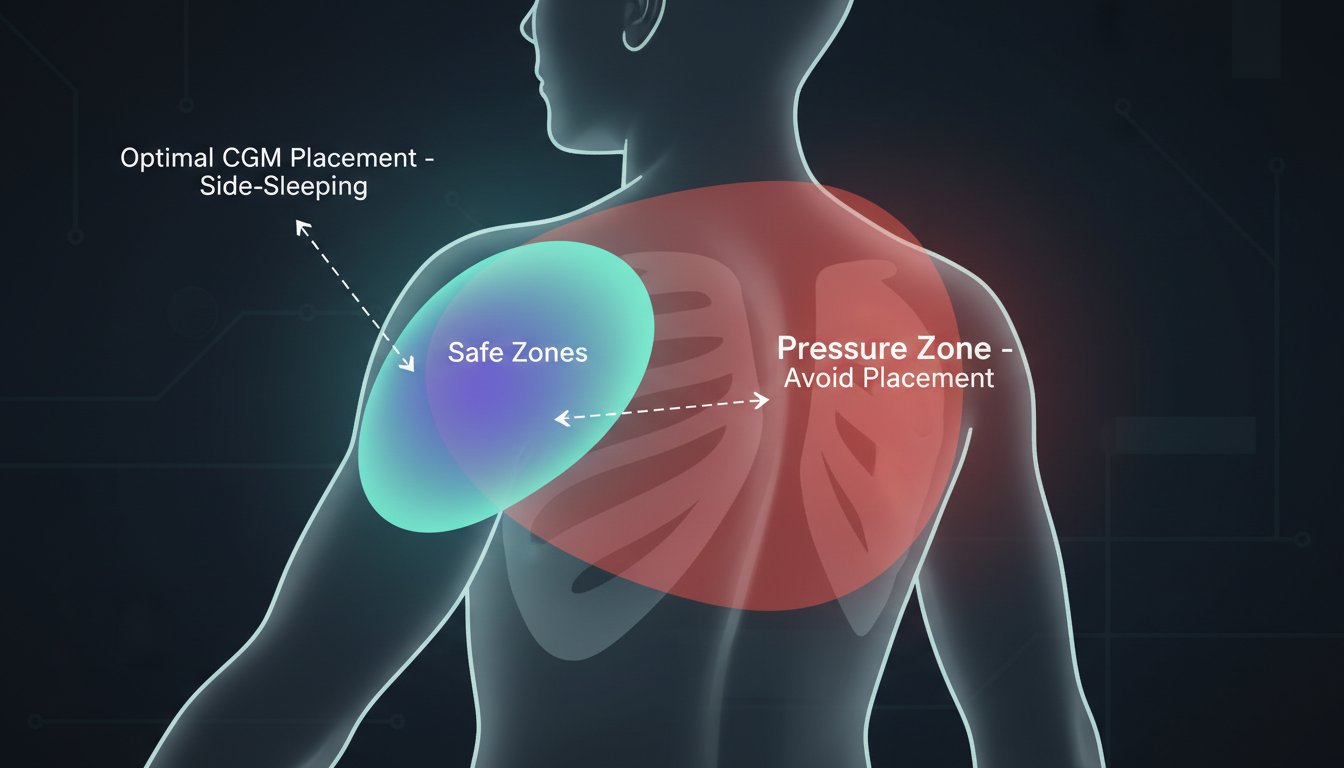
Strategic Sensor Placement to Minimize Pressure
The most effective way to prevent compression lows is to choose a sensor site that is unlikely to be pressed against the mattress during your preferred sleeping position.
Know Your Sleep Style
If you are a side sleeper, placing the sensor on the back of your arm is a recipe for nighttime alarms. Every time you roll onto that side, you’ll trigger a drop.
- Back Sleepers: The back of the arms or the abdomen are generally safe.
- Stomach Sleepers: Avoid the abdomen; the back of the arms or the upper buttocks (if approved for your specific device) may be better.
- Side Sleepers: Try the "inner" part of the arm (though not too close to the armpit) or the front of the thigh.
The "Sweet Spot" on the Arm
Many people find success by moving the sensor slightly more toward the front or the very back of the arm, rather than directly on the lateral side. Before applying your next sensor, lay down in your bed in your most common sleeping positions. Note which parts of your body are making the most contact with the mattress. Mark the "empty" spaces with a skin-safe pen—these are your ideal sensor zones.
Always remember that while many users experiment with "off-label" sites like the chest or thighs, you should consult your doctor or the device manufacturer's guidelines before trying a new location to ensure the accuracy of your readings.
Sleep Gear and Hygiene for Success
Sometimes, even the best placement can't prevent a roll in the middle of the night. This is where physical barriers and sleep hygiene come into play.
Using Overpatches and Protective Covers
A simple overpatch can help keep the sensor stable, but for compression lows, look for "sensor shields" or hard-shell covers. These are plastic caps that fit over the sensor and distribute the pressure onto the surrounding skin rather than directly onto the sensor itself. This keeps the interstitial fluid flowing even if you lean on the area.
The Power of the Body Pillow
If you are a side sleeper who struggles to stay off your sensor, a body pillow is a game-changer. By hugging a long pillow, you create a physical barrier that prevents you from rolling fully onto your stomach or the opposite side. It also helps align your spine, which provides additional health benefits.
Strategic Clothing
Loose, silky pajamas can sometimes cause the sensor to snag, while very tight clothing can add to the compression. Many CGM users find that wearing a snug (but not restrictive) t-shirt or an armband designed for glucose monitors helps keep the sensor in place and provides a small amount of cushioning against the bedsheets.
How to Spot a Compression Low in Real-Time
Learning to read the "shape" of your glucose graph can help you distinguish a real emergency from a false alarm. A glucose tracking app like GlucoAI can be incredibly helpful here, as it allows you to look at historical patterns and see how your body typically responds to nighttime lows.
The "Cliff" vs. The "Slope"
- Real Hypoglycemia: Usually appears as a gradual decline. Your blood sugar might move from
110to95to80to65over the course of 30 to 60 minutes. - Compression Low: Often looks like a vertical drop, sometimes called a "cliff." You might go from a stable
105to55in a single 5-minute reading.
The Quick Recovery
When you roll off a sensor, the reading usually "rebounds" almost as quickly as it dropped. If you see a sudden drop followed by a sudden return to your previous baseline without eating any carbs, it was almost certainly compression.
The "Feel" Test
Never ignore how you feel, but also don't rely on it entirely. If the CGM says you are at 50 mg/dL but you feel energetic and clear-headed, stay calm. Take a deep breath, sit up, and perform a manual finger-prick test. Always confirm with a blood glucose meter before treating a suspected nighttime low.
Managing Alarms and Regaining Peace of Mind
If compression lows are ruining your sleep, you might need to adjust your alert settings. Most modern diabetes management tools allow you to customize your "Low" threshold.
If your doctor agrees, you might consider setting your nighttime low alert slightly lower (for example, at 70 mg/dL instead of 80 mg/dL) to reduce "nuisance" alarms, provided it is safe for your specific health profile. Some apps also allow you to set a "snooze" or a delay for alerts, though this should be used with extreme caution.
Using a comprehensive glucose tracking app can help you document these events. By tagging a drop as a "compression low" in your logs, you can provide your healthcare provider with a clearer picture of your actual metabolic health, ensuring that these false data points don't skew your Time in Range or Glucose Management Indicator (GMI) reports.
Summary
Compression lows are a frustrating but manageable part of living with CGM technology. By understanding that physical pressure—not just insulin or food—affects your readings, you can take control of your nighttime experience.
Key Takeaways:
- Understand the Fluid: Remember that CGMs measure interstitial fluid; pressure pushes this fluid away, causing false low readings.
- Identify the "Cliff": Look for sudden, vertical drops on your graph as a sign of a compression low.
- Strategize Placement: Use "dry runs" in bed to find body areas that don't touch the mattress.
- Verify Before Treating: Always use a finger-prick meter to confirm a low before consuming rescue carbs.
- Optimize Your Gear: Consider body pillows or protective sensor shields to maintain a physical buffer.
- Consult Professionals: Always talk to your doctor before changing your alert settings or testing new sensor sites.
Managing your glucose shouldn't mean sacrificing your sleep. With a few tactical adjustments to your routine and a better understanding of your data, you can silence the false alarms and wake up feeling truly refreshed.
If you're looking for a better way to track these patterns and gain deeper insights into your glucose health, consider using a tool designed to make sense of the data. Managing your metabolic health is a journey—let's make it a well-rested one.
Ready to take the guesswork out of your glucose data? Download GlucoAI today to start tracking your trends and optimizing your metabolic health with ease!
GlucoAI — Smart Blood Sugar Monitor
Track, analyze, and optimize your glucose levels with AI-powered insights.