- Published on
Preparing for Your Doctor Visit with CGM Data
Have you ever walked into your doctor’s office, sat down on that crinkly paper-covered exam table, and suddenly forgotten every question you meant to ask? You aren't alone. For many of us living with diabetes or monitoring our metabolic health, those 15 to 20 minutes with a healthcare provider can feel like a high-pressure sprint. You want to show your progress, but explaining weeks of finger-prick logs or "feeling" like your sugar is high doesn't always paint the full picture.
This is where your Continuous Glucose Monitor (CGM) becomes your best advocate. Unlike a single A1C (average blood sugar level over 3 months) test, which provides a long-term average, your CGM data tells a story. It shows the peaks, the valleys, and the "why" behind your numbers. However, handing your phone to your doctor and saying, "Look at all these lines!" isn't the most effective strategy. To get the most out of your visit, you need to translate that raw data into actionable insights.
Preparing your CGM data before you step into the clinic transforms you from a passive patient into an active partner in your care. Let's walk through a five-step guide to help you prepare for your next appointment like a pro.
Step 1: Focus on the "Big Picture" Metrics
Before diving into specific daily spikes, start with the high-level metrics that doctors use to assess your overall management. While the A1C remains a gold standard for many providers, the medical community is increasingly prioritizing "Time in Range" (TIR).
Time in Range refers to the percentage of time your glucose levels stay within your target window—usually between 70 and 180 mg/dL. Research shows that increasing your TIR is closely linked to a lower risk of long-term complications. Along with TIR, you should look at your Glucose Management Indicator (GMI). This is an estimate of what your A1C might be based on your CGM data.
Another critical metric is your "Glucose Variability," often expressed as a percentage called the Coefficient of Variation (%CV). This measures how much your sugar swings. A lower percentage (ideally under 36%) means your levels are stable, whereas a higher percentage suggests "glucose rollercoasters" that can be exhausting and difficult to manage.

Step 2: Identify Your Most Frequent Patterns
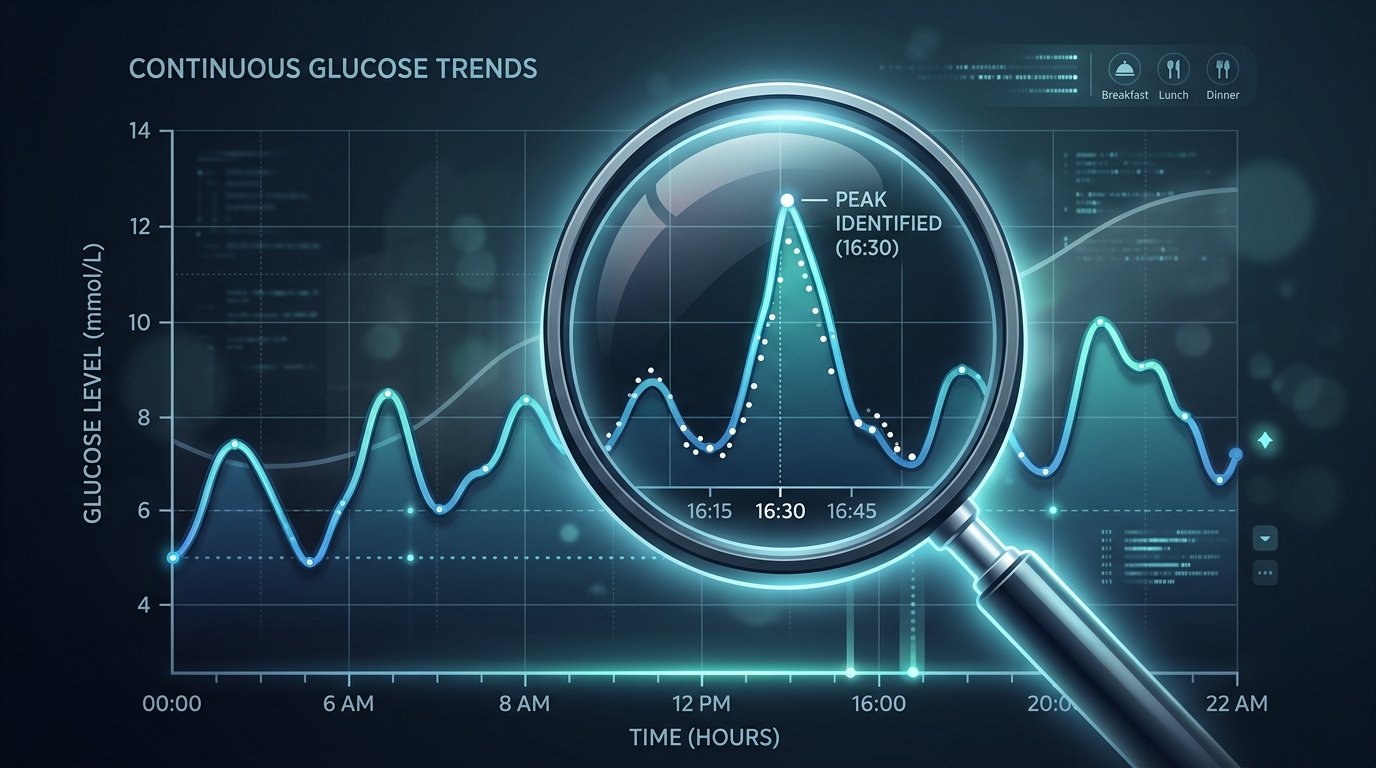
Data is only useful if it reveals a trend. Instead of looking at every single day, look for "the rule, not the exception." Most CGM software and glucose tracking apps allow you to view an Ambulatory Glucose Profile (AGP). This report overlays multiple days of data to show where your glucose typically sits at different times of the day.
Ask yourself these three questions while reviewing your AGP:
- The Overnight Trend: Does my glucose stay stable while I sleep, or does it steadily rise? (This could indicate the "Dawn Phenomenon" or a need for basal insulin adjustment).
- The Post-Meal Peak: Which meal consistently causes the highest spike? Is it breakfast, lunch, or dinner?
- The "Lows": Am I experiencing hypoglycemia (low blood sugar) at the same time every day, such as mid-afternoon or right after exercise?
Identifying these patterns allows you to say to your doctor, "I’ve noticed that I consistently spike to 220 mg/dL after breakfast," which is much more helpful than saying, "I think my breakfast is a problem."
Step 3: Connect the Dots with Lifestyle Context
Raw CGM data tells your doctor what happened, but your lifestyle logs tell them why. A spike to 200 mg/dL looks bad on a graph, but if that spike happened because you were fighting a head cold or under a massive deadline at work, the clinical response is very different than if it happened while you were fasted.
In the week leading up to your appointment, be extra diligent about logging context. This includes:
- Food: You don't necessarily need to count every calorie, but note high-carb meals or "trigger foods."
- Exercise: Note the type of workout. Did a HIIT session cause a temporary spike? Did a long walk cause a late-night drop?
- Stress and Sleep: High cortisol from stress or a poor night's sleep can significantly raise insulin resistance.
- Medication: Ensure you are logging exactly when you take your doses.
Using a comprehensive tool like GlucoAI can help you bridge this gap by keeping your glucose data and lifestyle notes in one place. When you can show your doctor that your "unexplained" spikes actually correlate with high-stress meetings, you can discuss stress management rather than just increasing medication.
Step 4: Curate Your "Top 3" Concerns
Doctors are often pressed for time. If you bring a list of 20 questions, you likely won't get through them all, or the answers will be rushed. Instead, use your CGM data to narrow your focus to your top three concerns.
Prioritize your concerns based on safety and quality of life. For example:
- Safety First: "I am having three unexplained lows per week at 2:00 AM. How can we prevent these?"
- Management Hurdles: "My glucose stays high for four hours after dinner despite my current medication. Should we adjust the timing?"
- Future Goals: "I want to start training for a 5K. How should I adjust my glucose management for increased activity?"
By leading with your most important data-backed concerns, you ensure that the most critical issues are addressed before the clock runs out.
Step 5: Export and Share Your Reports Early
The most common "time-waster" in a doctor's visit is the first 10 minutes spent trying to sync a device, find a cable, or log into a portal. Technology is great until it doesn't work in the clinic's dead zone for Wi-Fi.
Most CGM systems allow you to share data directly with your clinic's portal. If yours doesn't, or if you prefer a more hands-on approach, export your data as a PDF report (specifically the AGP report) 24 to 48 hours before your visit. You can email this to the office or print a hard copy to bring with you.
When you arrive with a printed report in hand, you are signaling to your provider that you are engaged and prepared. This allows you to spend your time discussing solutions rather than troubleshooting technology.
Summary: Your Pre-Visit Checklist
Preparation is the key to moving from "managing" diabetes to "mastering" it. Here are the key takeaways to remember for your next visit:
- Know your numbers: Be ready to discuss your Time in Range (TIR) and GMI.
- Spot trends: Look for recurring highs or lows at specific times of day.
- Provide context: Use your lifestyle logs to explain "outlier" data points.
- Prioritize: Select your top three concerns to ensure they get the attention they deserve.
- Share early: Send your reports or print them out before you arrive.
Please consult your doctor before making any changes to your medication or treatment plan based on your CGM data. Your healthcare provider is your partner in interpreting these numbers safely.
Ready to take the stress out of data tracking? Start using GlucoAI today to sync your CGM data, log your meals, and generate the insights you need for a more productive doctor's visit. Small steps in preparation lead to big wins in your health journey!
GlucoAI — Smart Blood Sugar Monitor
Track, analyze, and optimize your glucose levels with AI-powered insights.