- Published on
Managing Reactive Hypoglycemia: Causes and Solutions
Have you ever finished a satisfying meal, only to feel shaky, dizzy, or incredibly tired just a few hours later? While we often focus on keeping blood sugar levels from going too high, experiencing a sudden drop after eating—a condition known as reactive hypoglycemia—can be just as challenging to manage.
Reactive hypoglycemia, sometimes called postprandial hypoglycemia, occurs when your blood glucose (the primary source of energy for your body) drops below normal levels within a few hours of eating a meal. It is a common experience for many people, even those who do not have a formal diagnosis of diabetes, but understanding why it happens is the first step toward reclaiming your energy and stability.
What Causes Reactive Hypoglycemia?
To understand reactive hypoglycemia, we first have to look at how your body processes carbohydrates. When you eat, your digestive system breaks down carbohydrates into glucose, which enters your bloodstream. In response, your pancreas releases insulin to help your cells absorb that glucose for energy.
In someone experiencing reactive hypoglycemia, this process sometimes goes into overdrive. Your body may release too much insulin in response to a meal, causing your blood sugar to plummet lower than necessary after the initial spike. Several factors can trigger this response:
- High-Glycemic Foods: Consuming meals heavy in refined sugars or processed carbohydrates causes a rapid spike in blood sugar. Your body reacts by overcompensating with a surge of insulin.
- Insulin Sensitivity: If your body is highly sensitive to insulin, even a moderate intake of carbohydrates can trigger a stronger-than-expected hormonal response.
- Meal Composition: A lack of protein, fat, or fiber in a meal means glucose enters your bloodstream very quickly. Without those "brakes," your blood sugar rises and falls much faster.
- Early Stages of Metabolic Dysfunction: Sometimes, reactive hypoglycemia can be an early indicator of insulin resistance or prediabetes, where the body struggles to regulate insulin secretion effectively.

Identifying the Symptoms
Recognizing the signs of a blood sugar dip is crucial for managing the condition effectively. Because these symptoms can manifest quite suddenly, keeping a log of how you feel after specific meals can provide valuable data. Common indicators include:
- Physical shakiness or trembling
- Sudden, intense hunger
- Heart palpitations or a racing pulse
- Difficulty concentrating or "brain fog"
- Sweating or feeling cold/clammy
- Unexplained irritability or anxiety
If you notice these patterns, it is a good idea to speak with your doctor. They can help rule out underlying medical issues and provide a clear diagnosis. Please consult your doctor before making significant changes to your diet or if you are concerned about persistent symptoms.
Practical Strategies for Stability
The goal of managing reactive hypoglycemia is to slow down the absorption of glucose. By creating a more gradual rise in blood sugar, you prevent the "over-correction" by your pancreas.
1. Focus on Nutrient Pairing
Never eat "naked" carbohydrates. If you are having a piece of fruit or a serving of oats, always pair it with a source of protein and healthy fat. For example, instead of just an apple, try an apple with a handful of almonds or a tablespoon of nut butter. The protein and fat slow down gastric emptying, ensuring that glucose enters your system at a manageable pace.
2. Prioritize Fiber
Fiber is a game-changer for glucose regulation. Soluble fiber, found in foods like chia seeds, flaxseeds, beans, and certain vegetables, forms a gel-like substance in the gut that delays digestion. By adding more non-starchy vegetables and legumes to your plate, you can significantly reduce the magnitude of your post-meal glucose spikes.
3. Change Your Eating Order
Research suggests that the order in which you eat your food matters. Try eating your vegetables and protein first, and saving your carbohydrates for the end of the meal. This simple habit can lead to a more stable glucose response compared to eating starches on an empty stomach.
4. Optimize Meal Frequency
For some, three large meals a day cause too much of a glucose swing. If you find yourself experiencing crashes, try smaller, more frequent meals that balance macronutrients. This can keep your energy levels steady throughout the day without overloading your system.
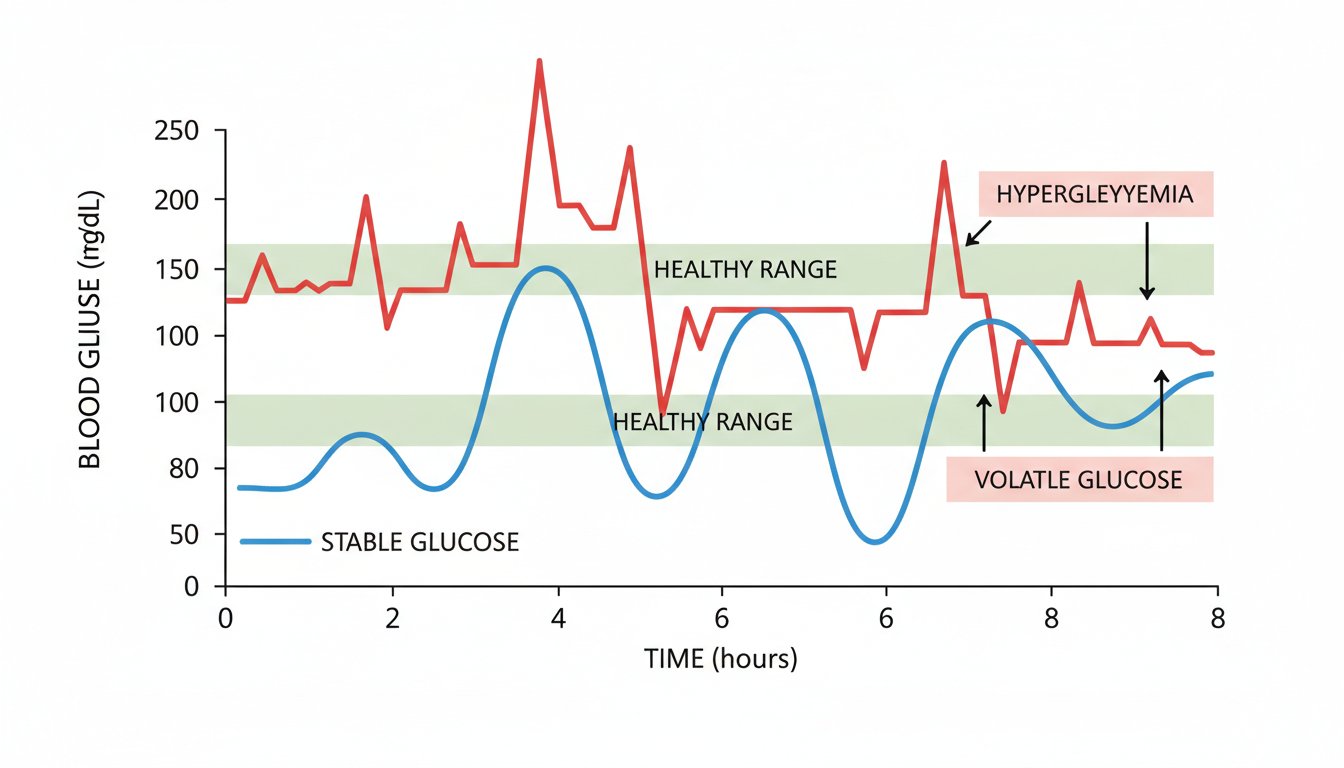
Tracking Your Progress with Data
Managing reactive hypoglycemia is difficult if you are guessing how your body is responding to different foods. This is where modern glucose monitoring tools become invaluable. By using a continuous glucose monitor (CGM) or regular blood glucose meter, you can see exactly how your body reacts to specific meals in real time.
Data-driven insights help you identify your "trigger foods"—those specific ingredients or meal combinations that consistently lead to a crash. Once you identify these patterns, you can adjust your diet with precision rather than relying on trial and error.
GlucoAI is designed to help you make sense of this data. By logging your meals and monitoring your glucose trends, you can visualize how different food choices impact your metabolic health. Identifying the relationship between what you eat and how your blood sugar responds is the most effective way to prevent future episodes of hypoglycemia.
When to Seek Medical Advice
While dietary adjustments are often effective, it is essential to ensure that your symptoms are not related to other medical conditions. If you experience frequent, severe episodes of hypoglycemia, or if you feel faint or lose consciousness, seek immediate medical attention. Always work with your healthcare provider to create a personalized plan that fits your unique metabolic needs.
Summary
Reactive hypoglycemia is a manageable condition, but it requires a proactive approach to nutrition and lifestyle. By focusing on stabilizing your blood sugar through fiber, protein, and healthy fats, you can avoid the mid-afternoon crashes that sap your energy.
Key Takeaways:
- Slow down the spike: Always pair carbohydrates with protein and fats to prevent rapid glucose absorption.
- Listen to your body: Keep track of when you feel shaky or tired to identify which meals might be causing a crash.
- Use technology: Utilize glucose tracking tools to gain objective insights into your body's unique response to different foods.
- Stay consistent: Small, sustainable dietary changes yield the best long-term results for metabolic stability.
If you are ready to take control of your metabolic health, start by tracking your meals and glucose levels consistently. Small, data-backed adjustments lead to significant improvements in how you feel every day. With the help of GlucoAI, you can turn your daily data into a clear roadmap for better health.
GlucoAI — Smart Blood Sugar Monitor
Track, analyze, and optimize your glucose levels with AI-powered insights.